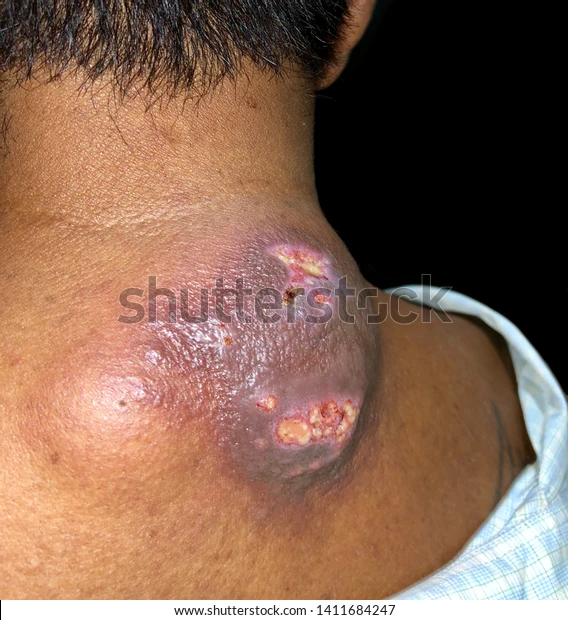
The aspiration of pus results in a noticeable and immediate improvement in the patient’s condition. The pressure caused by the abscess is relieved, leading to a reduction in pain and swelling. This provides rapid symptom relief and helps the body begin the healing process. In many cases, the procedure can be performed in a clinical setting under local anesthesia, with the patient often feeling significant comfort soon after the procedure.
Lymph nodes play an important role in the development of abscesses. These small, bean-shaped glands are part of the body’s immune system and are responsible for filtering harmful substances, including bacteria. Infections or inflammation in the body can cause lymph nodes in the neck area to become swollen and painful, a condition known as lymphadenitis. In some instances, the infection can spread, leading to the formation of a cold abscess—a non-purulent, often sterile collection of fluid that may develop around the lymph nodes.
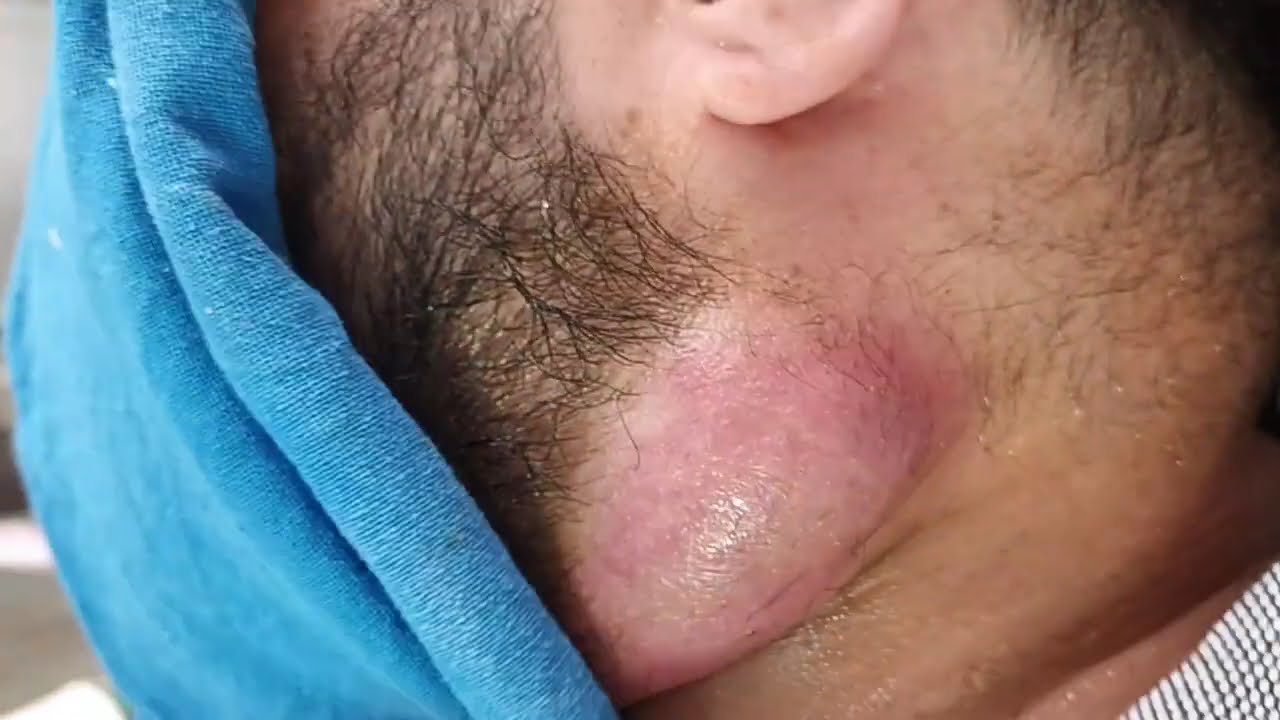
Cold abscesses are typically seen in chronic infections and present as painless, soft lumps in the neck. Unlike typical abscesses, they do not produce pus. Treatment for cold abscesses may involve drainage, antibiotics, and sometimes surgery, depending on the severity of the infection. Early detection and treatment are critical for the successful resolution of any abscess.
What is a Giant Neck Abscess?
A neck abscess is a localized collection of pus in the neck due to infection. It is typically caused by bacteria, although it can also be due to fungal or viral infections. In some cases, the infection may arise from nearby structures such as the teeth (dental abscess), tonsils (peritonsillar abscess), or the sinuses. A giant neck abscess refers to a large, significant collection of pus that causes considerable swelling and discomfort, often extending beyond the normal limits of the neck structures.
Causes and Risk Factors:
-
Bacterial Infection:
-
Staphylococcus aureus (including Methicillin-resistant Staphylococcus aureus [MRSA]) is one of the most common causative agents.
-
Streptococcus species can also be responsible, particularly in patients with tonsillar or dental infections.
-
-
Dental Infections: A dental abscess, if left untreated, can spread into the neck.
-
Tonsillar and Pharyngeal Infections: Chronic or severe tonsillitis or a peritonsillar abscess can lead to an infection in the deep neck spaces.
-
Trauma: A wound or foreign body penetration can provide an entry point for bacteria, leading to abscess formation.
-
Immunocompromised States: Patients with diabetes, cancer, or those on immunosuppressive therapy are at a higher risk for developing neck abscesses.
Clinical Presentation:
The clinical signs of a giant neck abscess include:
-
Severe neck pain and tenderness
-
Swelling of the neck that may be asymmetrical, sometimes with visible fluctuation
-
Fever and chills
-
Difficulty swallowing (dysphagia) and/or breathing (dyspnea)
-
Trismus (difficulty opening the mouth due to pain)
-
Signs of systemic infection such as lethargy, malaise, or confusion (particularly in severe cases)
Diagnosis:
-
Physical Examination:
-
A detailed physical exam will reveal the size, consistency, and location of the abscess.
-
The presence of fluctuance (a feeling of fluid under the skin) is a key sign suggesting the collection of pus.
-
-
Imaging:
-
Ultrasound: Often the first step in diagnosis to assess the abscess and guide needle aspiration.
-
CT Scan: Computed tomography with contrast is particularly helpful in identifying the size, extent, and anatomical location of deep neck abscesses. It can also reveal associated complications such as airway compromise.
-
MRI: May be used in complex cases, particularly when there is concern about involvement of deep spaces in the neck (e.g., retropharyngeal abscess).
-
-
Laboratory Tests:
-
Blood cultures can help identify the causative organism.
-
Aspiration or Drainage: Pus from the abscess can be sent for culture and sensitivity testing to identify the specific pathogen and guide antibiotic treatment.
-
Treatment:
-
Antibiotic Therapy:
-
Initial Empiric Antibiotics: Broad-spectrum antibiotics, such as intravenous (IV) ceftriaxone or cefotaxime combined with metronidazole, are often used to cover common pathogens (Streptococcus and Staphylococcus species, including MRSA).
-
Tailored Antibiotics: Once the specific bacteria are identified from culture, antibiotics may be adjusted to target the particular pathogen.
-
-
Surgical Intervention (Drainage):
-
Incision and Drainage (I&D): The primary treatment for a giant neck abscess is surgical drainage. This involves making an incision in the skin over the abscess and draining the pus to relieve pressure and clear the infection. Drainage is often done in the operating room under sterile conditions to reduce the risk of contamination.
-
Deep Neck Space Abscesses: Abscesses in the deeper neck spaces may require more invasive surgical drainage or even involvement of an otolaryngologist (ENT specialist) or a surgeon.
-
-
Postoperative Care:
-
The wound is typically packed with sterile gauze to promote continuous drainage and prevent premature closure.
-
The patient may require suction drainage if there is significant pus production.
-
Follow-up imaging may be necessary to ensure complete resolution of the abscess.
-
-
Pain Management:
-
Analgesics such as acetaminophen or ibuprofen are often used for pain relief.
-
In more severe cases, narcotic analgesics may be required, particularly after drainage.
-
-
Monitoring for Complications:
-
Airway Obstruction: In cases of massive swelling or involvement of the retropharyngeal or peritracheal spaces, there is a risk of airway obstruction, which requires urgent management (e.g., intubation or tracheostomy).
-
Sepsis: Giant neck abscesses can lead to sepsis, a life-threatening systemic infection, requiring urgent broad-spectrum IV antibiotics and intensive monitoring in an ICU if necessary.
-
Recurrent Infection: In some cases, the abscess may recur, and further drainage may be required.
-
Prognosis:
-
With prompt treatment (drainage and antibiotics), the prognosis for a giant neck abscess is generally good. However, if left untreated, it can lead to severe complications such as airway obstruction, sepsis, or the spread of infection to adjacent structures (e.g., mediastinum, brain).
References:
-
DeAngelis, M. (2017). “Deep Neck Infections.” In: Hematology/Oncology Clinics of North America, 31(3): 533-550.
-
This article provides a comprehensive overview of the pathophysiology, clinical presentation, and treatment of deep neck infections, including abscesses.
-
-
McKinney, P. M., & Fried, M. P. (2008). “Deep Neck Infections.” In: Otolaryngology-Head and Neck Surgery, 139(4): 489-493.
-
This review focuses on the evaluation and management of deep neck infections, including surgical strategies and complications.
-
-
Koehler, P. A., & Ewing, L. M. (2016). “Management of Neck Abscesses in Adults.” In: Emergency Medicine Clinics of North America, 34(3): 359-374.
-
This clinical article covers the epidemiology, diagnosis, and treatment options for neck abscesses, with an emphasis on emergency management.
-
-
Chung, S. E., & Liu, D. T. (2015). “Peritonsillar and Parapharyngeal Abscesses in Children and Adults.” In: Journal of Otolaryngology, 44(2): 182-188.
-
A detailed review of peritonsillar and deep neck abscesses, with a discussion on management strategies and complications.
-