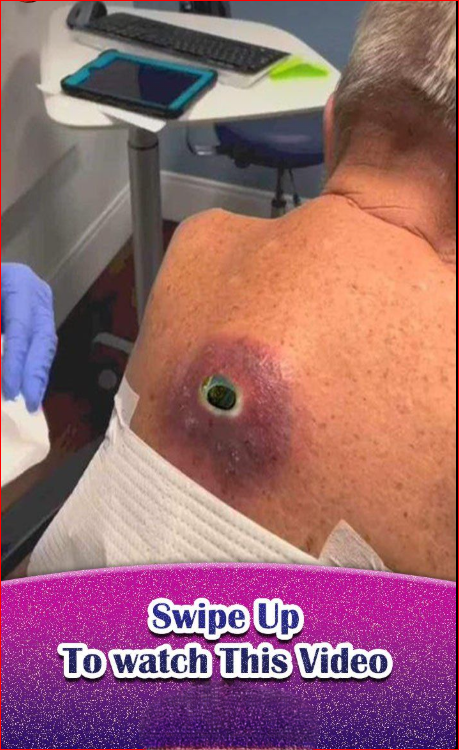
A giant abscess is a collection of pus that forms in a body part due to an infection, and it’s typically much larger than a standard abscess. They can occur anywhere in the body but are most commonly found in the skin, under the skin, or in internal organs. Here’s a breakdown of how an abscess, including a giant one, forms and the factors that may contribute to it:
How Abscesses Form:
-
Infection: An abscess generally forms when bacteria (such as Staphylococcus aureus) enter the body through a break in the skin, an infection in an organ, or even a blocked gland. The body’s immune system responds to the infection by sending white blood cells to fight the bacteria, which causes the tissue to become inflamed.
-
Pus Formation: The body produces pus as part of its defense mechanism. Pus consists of dead cells, bacteria, and tissue debris. This pus accumulates in a pocket, forming an abscess.
-
Abscess Expansion: Over time, if the infection isn’t addressed, the abscess can grow larger, forming a “giant” abscess. The infection may spread, causing the abscess to grow rapidly and potentially cause further complications.
Common Causes of Giant Abscesses:
-
Bacterial Infections:
- Staphylococcus aureus is a common cause, including MRSA (Methicillin-resistant Staphylococcus aureus), which can lead to more severe abscesses.
- Dental abscesses or abscesses related to an infected tooth can also become large if not treated.
-
Blocked Glands or Hair Follicles: Blockages in sweat glands, sebaceous glands (such as in acne), or hair follicles can create pockets of infection. If these get infected, they can develop into larger abscesses.
-
Poor Immune Response: Conditions like diabetes, immunosuppressive therapy, or compromised immune systems can make individuals more prone to developing large abscesses because the body has a harder time fighting off infections.
-
Trauma or Injury: An injury that allows bacteria to enter the body, particularly deep wounds, can develop into a large abscess if not cleaned and treated properly.
-
Infected Foreign Bodies: If a foreign body (like a splinter, catheter, or surgical implant) becomes infected, it can lead to an abscess.
-
Chronic Infections: If an infection is recurrent or left untreated for a long time, it can lead to the formation of a giant abscess.
Symptoms of a Giant Abscess:
- Pain: Abscesses are typically painful, and the pain worsens as the abscess grows.
- Redness and Swelling: The area around the abscess will usually become inflamed, red, and swollen.
- Warmth: The infected area may feel warm or hot to the touch.
- Fever: In severe cases, an abscess can cause a fever as the body fights the infection.
- Pus Drainage: If the abscess bursts, you may notice yellow or green pus draining from the wound.
- Larger Abscesses: Giant abscesses may be visibly large, and in severe cases, they can cause structural damage or affect nearby tissues and organs.
Treatment of a Giant Abscess:
-
Drainage: The most common treatment for an abscess is drainage. This is typically done by a healthcare professional who will cut open the abscess and drain the pus.
- Incision and Drainage (I&D) is a procedure in which a small incision is made to allow the pus to escape, and the abscess cavity is cleaned.
-
Antibiotics: After draining, antibiotics are often prescribed to treat the underlying bacterial infection. The choice of antibiotic will depend on the type of bacteria causing the abscess.
- In the case of MRSA or other resistant bacteria, specific antibiotics like vancomycin or clindamycin may be used.
-
Warm Compresses: Applying a warm compress to the abscess may help reduce swelling and pain, and encourage it to drain naturally, although this is typically only for smaller abscesses.
-
Surgical Removal: In some cases, especially with large or recurring abscesses, surgical removal may be necessary to ensure the infection is completely cleared.
-
Follow-Up Care: After treatment, follow-up care is essential to monitor for signs of recurrence or complications like infection spreading to surrounding tissues or the bloodstream (sepsis).
Prevention:
- Good Hygiene: Keeping the skin clean and avoiding injuries can reduce the risk of infections that lead to abscesses.
- Proper Wound Care: Cleaning and covering cuts, burns, or other injuries promptly can prevent bacteria from entering and causing an infection.
- Managing Chronic Conditions: For individuals with diabetes or other conditions that impair the immune system, it’s important to manage these conditions to reduce the risk of developing abscesses.