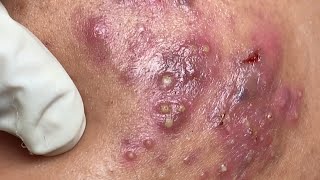
Incision and drainage (I&D) of a buccal space infection is a medical procedure that involves making a small incision in the skin or mucous membrane to allow pus or fluid to drain from an abscess, in this case, in the buccal space. The buccal space is located in the cheek region, which contains important structures such as muscles, blood vessels, and salivary glands.
Here is a general overview of how the procedure is performed:
Indications:
-
A buccal space infection often arises from dental abscesses, periapical infections, or infected salivary glands.
-
Symptoms may include swelling, pain, fever, and difficulty opening the mouth (trismus).
Preparation:
-
Assess the Patient:
-
Perform a thorough history and physical examination.
-
Confirm the diagnosis of a buccal space infection, often confirmed by imaging (such as an X-ray or CT scan).
-
Ensure the patient is stable and identify any contraindications to surgery.
-
-
Sterilization:
-
Perform hand hygiene and use appropriate personal protective equipment (PPE).
-
Sterilize the skin or mucosa around the infection site with antiseptic (e.g., chlorhexidine).
-
-
Local Anesthesia:
-
Use a local anesthetic (e.g., lidocaine) to numb the area.
-
In some cases, regional anesthesia may be necessary, depending on the extent of the infection.
-
Procedure:
-
Incision:
-
The typical approach is to make an incision inside the mouth (intraoral) along the buccal mucosa near the location of the abscess.
-
The incision should be made at the most fluctuant (softest, swollen) part of the abscess to maximize drainage.
-
A small scalpel (e.g., #11 blade) is used to make a vertical or horizontal incision in the buccal mucosa, depending on the size and location of the abscess.
-
-
Drainage:
-
Once the abscess cavity is exposed, the pus is allowed to drain freely.
-
The pus may need to be gently expressed by applying pressure around the area.
-
A Penrose drain or other soft drain may be inserted to maintain drainage for a few days and prevent the abscess from reforming.
-
-
Exploration:
-
Carefully explore the wound to ensure there are no remaining pockets of pus or debris.
-
In some cases, you may need to irrigate the cavity with saline to help clean out any residual infected material.
-
-
Hemostasis:
-
Control any bleeding using gentle pressure or cauterization if necessary.
-
-
Closure:
-
In most cases, the wound is left open to drain.
-
If the infection is controlled, the mucosal edges are often approximated with absorbable sutures (though this may not be necessary in all cases).
-
Post-Procedure Care:
-
Pain Management: Prescribe analgesics (e.g., ibuprofen or acetaminophen).
-
Antibiotics: Prescribe appropriate antibiotics to treat the infection. Typically, broad-spectrum antibiotics like amoxicillin-clavulanate or clindamycin are used.
-
Follow-up: Schedule a follow-up appointment to monitor the healing process, ensure adequate drainage, and address any complications like wound infection or recurrence.
-
Oral Hygiene: Instruct the patient to perform gentle oral hygiene and to avoid irritating the surgical site, particularly while eating or drinking.
Complications to Watch For:
-
Incomplete drainage or re-accumulation of pus.
-
Wound infection or cellulitis.
-
Severe swelling or airway compromise, especially if the infection spreads.
-
Damage to adjacent structures such as nerves (e.g., the facial nerve) or blood vessels.
Alternative Approaches:
-
In some cases, a facial incision (extraoral approach) may be necessary if the infection is large or difficult to drain from the inside of the mouth.
Conclusion:
Incision and drainage of a buccal space infection is a routine but important procedure to manage abscesses in the cheek region. The procedure should be done with care, considering the potential for complications, especially with airway management. Proper post-procedure care is essential for a successful recovery.
Detailed Procedure of Incision and Drainage of Buccal Space Infection
Anatomy and Pathophysiology of the Buccal Space:
The buccal space is part of the facial space located in the lateral aspect of the face and contains the buccinator muscle, part of the parotid gland, the facial artery, and branches of the trigeminal nerve. Infections in this area typically originate from dental abscesses or other infectious processes like periapical infections, periodontal abscesses, or salivary gland infections. These infections can present with localized pain, swelling, fever, and difficulty opening the mouth (trismus). If left untreated, the infection may spread to surrounding spaces and even cause sepsis.
Indications for Incision and Drainage (I&D):
-
Fluctuant swelling (indicating an abscess).
-
Failure to improve with antibiotics or drainage via conservative methods.
-
Persistent pain in the buccal area.
-
Systemic signs of infection such as fever or malaise.
-
Complications like airway obstruction or cellulitis.
Pre-Procedure Considerations:
-
Assessment: A detailed clinical examination is performed to localize the abscess. Imaging such as dental X-rays or a CT scan may be necessary to determine the exact extent and location of the infection.
-
Lab Workup: While not always necessary, blood tests (CBC, CRP) can provide information about systemic infection.
-
Patient Preparation:
-
Anesthesia: Local anesthesia (e.g., 1% lidocaine with epinephrine) is used for the procedure. Depending on the patient’s anxiety, conscious sedation may be administered.
-
Sterilization: Thorough cleaning of the oral cavity and external skin (if needed) is done to reduce bacterial contamination.
-
-
Antibiotics: Typically, broad-spectrum antibiotics (e.g., amoxicillin-clavulanate, clindamycin, or metronidazole) are given prior to the procedure if the infection is severe or has spread.
Step-by-Step Procedure of Incision and Drainage:
-
Positioning and Preparation:
-
The patient is positioned in a supine or reclined position, ensuring easy access to the buccal area.
-
Use sterile drapes to cover the patient’s face and neck.
-
Apply a sterile towel around the operative area to reduce contamination risk.
-
-
Injection of Local Anesthetic:
-
Inject the anesthetic into the buccal mucosa along the planned incision line. This is done with a fine needle to ensure proper numbing of the area.
-
-
Making the Incision:
-
The incision is typically made inside the cheek along the most fluctuant (soft and swollen) part of the infection. A small vertical or horizontal incision is preferred to avoid damage to important facial structures (e.g., nerves, blood vessels).
-
Scalpel (usually #11 or #15 blade) is used to make the incision. The incision should be about 1-2 cm in length.
-
-
Drainage:
-
Upon incision, pus will drain freely from the abscess cavity.
-
The cavity should be gently squeezed to express any remaining pus.
-
If necessary, irrigation with saline or an antiseptic solution (e.g., chlorhexidine) can be used to clean the cavity and reduce bacterial load.
-
-
Exploration:
-
Using a sterile instrument (e.g., hemostat), explore the cavity to check for any remaining pus or loculations (pockets of infection). This ensures complete drainage.
-
A Penrose drain or rubber drain may be placed into the cavity to promote continued drainage over the next 24-48 hours.
-
-
Hemostasis:
-
Control any bleeding with gentle pressure, and if needed, apply a hemostatic agent.
-
-
Closure:
-
In most cases, the wound is left open to allow continued drainage.
-
If the infection is well controlled, the edges of the mucosal incision may be approximated with absorbable sutures (e.g., Vicryl).
-
A small, non-absorbable drain may be used to facilitate drainage if needed.
-
-
Post-Procedure Care:
-
The patient is usually given analgesics (e.g., ibuprofen or acetaminophen) for pain relief.
-
Antibiotics are continued for several days to address the underlying infection.
-
Oral hygiene instructions should be given, emphasizing gentle mouth rinses (e.g., saline or chlorhexidine) and avoiding mechanical irritation.
-
Post-Procedure Management:
-
Pain Control: Over-the-counter analgesics (e.g., acetaminophen, ibuprofen) or prescription pain relief can be provided as necessary.
-
Antibiotics: Continue antibiotics as prescribed, and tailor to culture and sensitivity results if available.
-
Follow-up: The patient should be seen in 24-48 hours for evaluation of drainage, signs of further infection, and removal of the drain (if placed).
-
Wound Care: Patients should avoid chewing or touching the incision site to prevent irritation or secondary infection.
Potential Complications:
-
Incomplete Drainage: If the abscess is not adequately drained, it may refill, necessitating further surgical intervention.
-
Wound Infection: The wound may become infected, requiring drainage or a change in antibiotics.
-
Damage to Adjacent Structures: Damage to the facial nerve, parotid duct, or other adjacent structures can occur if proper care is not taken during the incision.
-
Recurrence: In some cases, the abscess may recur if not entirely drained.
References and Guidelines:
-
Kaufman, E. et al. (2019). “Dental Abscess and Buccal Space Infections: A Review of Management.” Journal of Oral and Maxillofacial Surgery. Link to journal article.
-
Tunkel, D.E., et al. (2020). “Management of Oral and Dental Infections.” American Family Physician. Link.
-
Ghali, G.E., et al. (2016). “Management of Facial Space Infections.” Oral and Maxillofacial Surgery Clinics of North America. Link.
These sources discuss the management, procedural techniques, and indications for I&D of abscesses in the oral cavity, specifically focusing on buccal space infections. You can look up these references for more in-depth guidance and surgical insights.