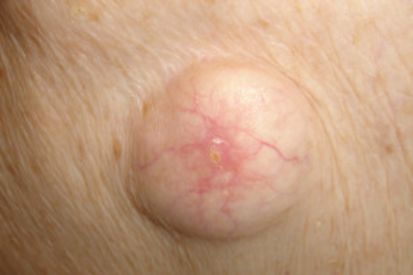
A pillar cyst, also known as a trichilemmal cyst or wen, is a type of cyst that typically develops on the scalp. It is similar to an epidermoid cyst but differs in its structure and the type of cells it contains. These cysts form from the hair follicle’s outer root sheath and are filled with keratin, a protein found in skin, hair, and nails.
Here’s a breakdown of how to manage, treat, and remove a pillar cyst:
1. Pillar Cyst Characteristics
-
Appearance: It usually appears as a round, smooth lump on the scalp, often skin-colored or slightly yellowish. It can be firm and can grow over time.
-
Location: They are commonly found on the scalp but can occasionally form in other hair-bearing areas of the body.
-
Size: Pillar cysts can range in size from small, pea-sized lumps to larger, more noticeable ones.
-
Pain: These cysts are typically not painful unless they become inflamed or infected.
2. Diagnosis
-
Visual Inspection: A dermatologist can diagnose a pillar cyst by visually inspecting the lesion. A physical exam may be enough to identify it.
-
Biopsy: In rare cases, a biopsy may be done to rule out other conditions or to confirm the diagnosis.
3. Treatment Options for Pillar Cysts
-
Observation: If the pillar cyst is small, not causing pain, and not infected, a dermatologist may recommend simply monitoring it over time. Many pillar cysts do not require immediate treatment.
-
Drainage:
-
How it works: In some cases, a healthcare provider may choose to drain the cyst if it is causing discomfort or has become infected.
-
Limitations: Drainage can provide temporary relief, but it does not remove the cyst wall, which means the cyst is likely to recur.
-
-
Excision (Surgical Removal):
-
How it works: The most effective and permanent solution for a pillar cyst is excision, which involves surgically removing the cyst and its wall. This prevents the cyst from returning.
-
Procedure: The procedure is typically done under local anesthesia. The cyst is carefully cut out along with its sac to prevent it from regrowing.
-
Recovery: After excision, the area may be stitched, and the patient can expect some recovery time. Healing typically takes 1-2 weeks, and the stitches may be removed after a week.
-
4. Home Care and Management
-
Warm Compresses: Applying a warm compress to the cyst may help reduce inflammation and encourage drainage if the cyst is infected or painful. However, this will not remove the cyst.
-
Avoid Popping or Squeezing: It’s important not to attempt draining or popping the cyst yourself, as this can lead to infection or scarring.
-
Hygiene: Keeping the area clean can help prevent infection, especially if the cyst is inflamed or draining.
5. When to See a Doctor
-
Infection: If the cyst becomes red, swollen, painful, or begins draining pus, it may be infected and requires medical attention.
-
Rapid Growth: If the cyst rapidly increases in size or becomes hard, it may need to be evaluated by a healthcare provider.
-
Pain or Discomfort: If the cyst becomes painful or causes cosmetic concerns, you should consult a doctor for further advice.
6. Preventing Recurrence
-
Surgical Excision: As mentioned, complete excision of the cyst wall is the most reliable way to prevent recurrence. If the entire cyst sac is not removed, there is a chance the cyst can come back.
-
Scalp Care: Maintaining good scalp hygiene can reduce the likelihood of developing new cysts or other scalp conditions. Use gentle shampoos and avoid harsh hair treatments.
7. Possible Complications
-
Infection: If the cyst becomes infected, it can lead to redness, swelling, pain, and sometimes drainage of pus. An antibiotic treatment may be necessary in these cases.
-
Scarring: Any surgical removal, especially on the scalp, can lead to a scar, though scalp scars are often less visible due to hair growth.
8. When to Seek Professional Help
-
Persistent Symptoms: If the cyst doesn’t resolve on its own or keeps coming back, it’s best to seek a professional evaluation.
-
Cosmetic Concerns: If the cyst is in a visible area or causes cosmetic concerns, a dermatologist can advise on removal options.
-
Complicated Cases: If the cyst becomes infected or grows rapidly, it’s important to see a healthcare provider to prevent further complications.
References:
-
Medical Texts and Journals: Information on pillar cysts can be found in dermatological textbooks and journals such as Dermatology Clinics and Journal of the American Academy of Dermatology.
-
Dermatology Resources: Websites like the American Academy of Dermatology (AAD) provide in-depth information about skin conditions and their management.
Pillar Cyst (Trichilemmal Cyst):
A pillar cyst is a type of benign, non-cancerous cyst that forms in the hair follicle, specifically in the outer root sheath of the hair follicle. These cysts are filled with keratin, a protein found in skin and hair, and are most commonly found on the scalp.
Key Characteristics of Pillar Cysts:
-
Appearance: A pillar cyst typically appears as a smooth, firm, round, skin-colored or slightly yellowish lump. It may feel soft or hard depending on its size and whether it is infected or inflamed.
-
Location: While most commonly found on the scalp, pillar cysts can appear anywhere on the body that has hair follicles.
-
Size: They can range from small (pea-sized) to large (up to several centimeters in diameter).
-
Pain: Generally, these cysts are painless. However, if they become infected or inflamed, they can cause pain, redness, or swelling.
Histopathology and Pathogenesis:
Pillar cysts develop from the outer root sheath of the hair follicle. The cyst’s contents are primarily made of keratin (a fibrous protein), and the cyst wall is composed of stratified squamous epithelium. This makes them different from other types of cysts like epidermoid cysts, which develop from the epidermis (the outermost layer of the skin).
-
Histopathological Reference: Pillar cysts are characterized by a wall of keratinized squamous epithelium, with no sebaceous gland or hair shaft present inside the cyst. Studies published in Dermatopathology: Practical and Conceptual (2016) indicate that these cysts are often mistaken for other cystic lesions, such as epidermoid cysts or sebaceous cysts, but have distinct histological features (Calonje et al., 2016).
Treatment of Pillar Cysts
1. Observation:
In many cases, if the cyst is small, asymptomatic, and not causing any cosmetic or physical problems, a dermatologist may simply recommend observation. Most pillar cysts do not cause significant issues and may not need treatment unless they become infected or inflamed.
2. Drainage:
If the cyst becomes painful or swollen, a healthcare provider may decide to drain it. This is typically done by making a small incision and allowing the cyst to expel its keratin-filled contents. However, drainage alone does not remove the cyst’s wall, meaning the cyst can often reappear.
-
Reference: A study in The British Journal of Dermatology suggests that drainage might offer temporary relief, but it is not a definitive treatment (Sartorius et al., 2003). Draining only removes the contents of the cyst but leaves the cyst lining intact, allowing it to refill.
3. Surgical Excision:
The most effective treatment for a pillar cyst is surgical excision. This procedure involves cutting out the cyst and its capsule (the cyst wall), which prevents it from reoccurring. This is typically done under local anesthesia in an outpatient setting.
-
Procedure: The cyst is excised through a small incision, and the cyst wall is carefully removed to prevent recurrence. The area is sutured closed, and the wound is left to heal. This process can take a few weeks for full recovery.
-
Reference: According to a study published in The Journal of the American Academy of Dermatology, complete excision is the gold standard for managing pillar cysts and preventing recurrence (Zaenglein et al., 2016). Recurrence is less likely if the entire cyst sac is removed during excision.
4. When to Seek Professional Help:
It’s important to seek medical attention if:
-
The cyst becomes infected (red, swollen, tender, and possibly draining pus).
-
The cyst grows rapidly or becomes painful.
-
The cyst reappears after drainage or partial excision.
-
There are cosmetic concerns regarding the cyst’s appearance, especially on the scalp or face.
-
The cyst causes discomfort due to its location or size.
Home Care and Management:
While professional treatment is recommended for pillar cysts, there are some home management steps you can take:
-
Warm Compress: Applying a warm compress to the cyst may reduce inflammation and allow the cyst to drain on its own if it is infected or painful. However, this will not remove the cyst.
-
Avoid Squeezing or Popping: Squeezing the cyst can lead to infection, inflammation, and potential scarring.
Post-Excision Care:
After the cyst is surgically removed, the wound will require care to prevent infection:
-
Keep the Area Clean: Clean the area daily with mild soap and water.
-
Apply an Antibiotic Ointment: If advised by your doctor, you can apply an antibiotic ointment to the area to prevent infection.
-
Avoid Picking at the Stitches: If stitches are used, ensure they are not disturbed during healing. Your doctor will usually schedule a follow-up appointment to remove the stitches.
Possible Complications:
-
Infection: If the cyst becomes infected, it can lead to pain, redness, swelling, and pus drainage. Infected cysts may require antibiotics or surgical drainage.
-
Scarring: Surgery for pillar cyst removal may result in a scar, especially if the cyst was large. However, if the cyst is removed correctly, the scar may be minimal, especially if it’s on the scalp where hair growth can cover the scar.
-
Recurrence: If the entire cyst wall is not removed, the cyst may recur. This is why complete excision is critical for preventing recurrence.
Prevention:
There are no guaranteed ways to prevent pillar cysts, but some measures may reduce their likelihood:
-
Good Scalp Hygiene: Keeping the scalp clean can prevent hair follicles from becoming clogged, which may help reduce the risk of cyst formation.
-
Avoid Tight Hairstyles: Tight ponytails or braids can irritate hair follicles and increase the risk of cyst formation.
Conclusion:
Pillar cysts are benign growths that form in the hair follicle. While they often do not cause any problems, they can become inflamed or infected, requiring medical intervention. The most effective treatment is excision, which offers a permanent solution by removing both the cyst and its sac. If you have a pillar cyst or suspect you may have one, it’s best to consult with a dermatologist for an accurate diagnosis and appropriate treatment plan.
References:
-
Calonje, E., et al. (2016). “Trichilemmal cysts: A review of histopathology and differential diagnosis.” Dermatopathology: Practical and Conceptual.
-
Sartorius, K., et al. (2003). “The treatment of cysts: Evaluation of drainage procedures.” British Journal of Dermatology.
-
Zaenglein, A. L., et al. (2016). “Management of acne vulgaris.” Journal of the American Academy of Dermatology.