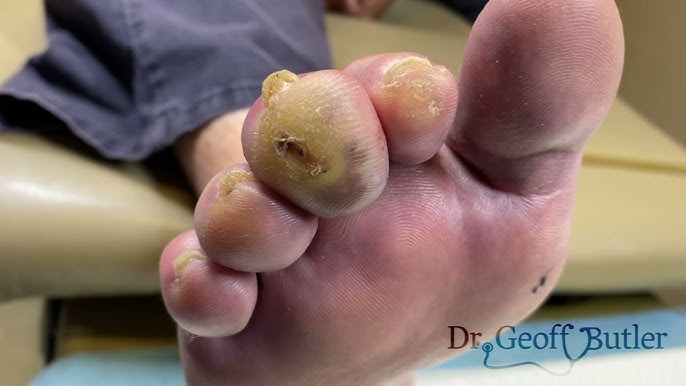
A foot abscess is a painful infection in the foot tissue often caused by bacteria, a virus, or a foreign substance. A pocket of pus usually develops, and the abscess appears red and swollen. A foot abscess can be a serious problem and worsen very quickly, often leading to potentially life-threatening consequences. If you are concerned that you may have a foot abscess, don’t delay scheduling an appointment with a podiatrist for diagnosis and treatment. 
The skilled foot doctors at Alliance Foot & Ankle Specialists in Tarrant County, Texas have experience diagnosing and treating abscesses and many other podiatric conditions. Here, our podiatrists discuss the symptoms of a foot abscess, the types of treatment options available, and what to do if you think you have developed an abscess.
Signs and Symptoms of a Foot Abscess
A foot abscess is a pocket of infection filled with pus that forms in the foot’s tissues. A foot abscess can develop when bacteria gets into a cut, puncture, or other type of wound that causes a break in the skin on your foot. Signs indicating a foot infection or abscess can vary depending on where the wound is located and how severe it is. Common symptoms of a foot abscess include the following:
- Localized pain. Throbbing or sharp pain is usually the first symptom of a foot abscess. The pain is often localized to the wound and may increase in intensity over time.
- Swelling. The affected area of the foot may become swollen as a result of inflammation caused by the infection.
- Tenderness. In addition to being painful and swollen, the skin over the wound may be tender to the touch.
- Warmth. The affected area may feel warmer to the touch than other parts of the foot.
- Redness. The skin around the wound may appear red or pink in color, due to increased blood flow to the area as the body works to fight the infection.
- Pus. As the infection progresses, pus (a yellowish or greenish fluid) may form within the foot wound.
- Difficulty walking. Depending on the position and size of the abscess, it may be difficult to walk or put weight on the affected foot.
- Fever. If the infection becomes severe or spreads, an individual with a foot abscess may develop a low-grade fever.
Patients with diabetes are at an elevated risk of developing hard-to-heal abscesses on their feet, but they are not the only ones at risk of developing foot ulcers. You should never ignore a foot wound. Whether you have diabetes or not, it’s critical to seek medical attention right away if you think you might have a foot abscess or any foot infection.
Seek Immediate Diagnosis and Treatment for a Foot Abscess
A foot abscess can worsen rapidly and create serious health issues, so it’s important to see a foot doctor right away for diagnosis and treatment. Waiting too long to see a podiatrist can lead to serious complications, such as a deeper tissue infection, the spread of infection, or even sepsis.
Diagnosing a Foot Abscess
When you come in for your podiatric appointment at Alliance Foot & Ankle Specialists, you’ll be able to have an open and honest discussion about your condition with Dr. Nichols or Dr. Harvey. The doctor you see will conduct a thorough examination and evaluation of your foot to determine if you have an abscess or if there is some other medical condition that needs treatment. The diagnostic process typically includes the following:
- Reviewing your medical history. Your podiatrist will ask about your symptoms and medical history to understand the context of the infection. You may have had a recent injury, stepped on a nail or foreign object, or suffer from a medical condition that increases your risk of developing foot ulcers, abscesses, or other foot conditions.
- Conducting a physical exam. Your foot doctor will examine the affected foot closely, looking for signs of redness, swelling, warmth, and tenderness. They may also look for visible wounds or cuts that could have served as an entry point for bacteria.
- Performing imaging tests. In some cases, your podiatrist may prescribe imaging tests, such as an X-ray or ultrasound, to assess the extent of the infection and determine if there are any underlying bone issues.
Treating a Foot Abscess
If the diagnostic exam indicates that you have a foot abscess, your foot doctor will recommend a treatment plan based on all of the information gleaned during the diagnostic process. Treating a foot abscess typically involves the following:
- Draining the abscess. Usually, the first step in treating a foot abscess is to drain the pus from the abscess. To do this, a foot doctor typically uses local anesthesia to numb the abscessed area before making an incision to drain the pus. In some cases, it may be necessary to leave a small rubber tube in place to allow for continued drainage.
- Wound care. Your treatment plan will require proper wound care, which is essential to promote healing and prevent further complications. Wound care for a foot abscess requires keeping the wound clean and covered, regularly changing the wound dressing, keeping pressure off the affected area, and following your foot doctor’s instructions.
- Antibiotics. Depending on the severity of the infection and your individual health factors, your doctor may prescribe antibiotics to help fight the bacterial infection and keep it from spreading or recurring. Oral antibiotics are often sufficient, although intravenous (IV) antibiotics can be needed in severe cases.
- Pain management. Your doctor may also prescribe pain relief medications to help you manage discomfort associated with the abscess and its treatment.
- Additional treatments. More extensive treatment or surgical intervention may be necessary if the abscess is very large or deep or there are complications, such as osteomyelitis (bone infection).
- Follow-up. Your podiatrist will recommend a follow-up schedule so they can monitor healing until the infection is fully resolved.
-
Injury or Break in the Skin: Any injury, cut, or break in the skin (even something as small as a blister or splinter) can allow bacteria to enter and multiply.
-
Bacterial Infection: Common bacteria, like Staphylococcus aureus, can cause an infection when they invade the area under the skin.
-
Infection and Inflammation: As the body tries to fight off the infection, the area becomes inflamed, swollen, and may feel warm or tender. The body creates pus to fight off the infection, and this pus builds up in a pocket beneath the skin, forming an abscess.
-
Symptoms: The foot will likely be painful, red, swollen, and may have a visible bump or lump. There may also be an increase in temperature and discomfort when touched.
1. Introduction of Bacteria or Pathogen
An abscess generally starts with the introduction of a pathogen (usually bacteria) into the body. This can happen in several ways, including:
- Cut, scrape, or puncture: A small injury, like stepping on a sharp object, or a cut from a toenail or another object, can provide bacteria an entry point into the skin.
- Ingrown toenails: This common condition happens when the edge of a toenail grows into the skin, creating an opening where bacteria can enter.
- Fungal infections: Conditions like athlete’s foot (caused by fungi) can compromise the skin, allowing bacteria to enter and cause an abscess.
- Pre-existing health conditions: Diabetes, poor circulation, and other conditions can increase the risk of infections and abscess formation.
2. Infection and Inflammatory Response
Once bacteria or other pathogens enter the skin, the immune system responds to contain the infection. The immune system sends white blood cells, such as neutrophils, to the site of infection. The inflammatory response leads to swelling, redness, warmth, and pain in the affected area. The body also forms a protective barrier around the infection to prevent the bacteria from spreading. This results in the formation of a pus-filled pocket within the skin.
- Pus consists of dead tissue, dead white blood cells, and bacteria that have been attacked by the immune system. This collection of fluid accumulates as the infection worsens.
3. Symptoms of Abscess Formation
As the abscess develops, the area becomes:
- Red, swollen, and warm: These are common signs of inflammation.
- Painful: Pressure from the pus buildup increases pain. The abscess may also become increasingly tender to the touch.
- Visible lump or bump: Depending on the size of the abscess, a visible bump or protrusion may form on the foot, sometimes with a white or yellow center where the pus is located.
- Fever: In more severe cases, the infection can cause a fever, a systemic response to the infection.
4. Risk Factors
Certain factors increase the risk of developing an abscess on the foot:
- Poor hygiene: Not keeping the feet clean and dry can create a favorable environment for bacterial growth.
- Diabetes: Individuals with diabetes are more prone to infections because high blood sugar can impair the immune response and cause poor circulation in the feet.
- Compromised immune system: Conditions such as HIV/AIDS, cancer treatments, and medications that suppress immunity (like steroids) can make it harder for the body to fight off infections.
- Chronic skin conditions: Conditions like eczema or psoriasis can break down the skin, providing an easy access point for bacteria.
- Tight shoes: Wearing shoes that are too tight or don’t fit properly can cause blisters, cuts, or other injuries that can lead to infections.
5. Diagnosis
A healthcare provider usually diagnoses an abscess based on the appearance of the foot and the symptoms you present. In some cases, a culture of the pus might be taken to identify the exact bacteria causing the infection, which helps determine the most appropriate antibiotic treatment. Imaging studies like an ultrasound may be used in more severe cases to assess the extent of the infection.
6. Treatment
Treatment typically depends on the severity of the abscess:
- Incision and drainage (I&D): The most common treatment for an abscess is a minor surgical procedure where the healthcare provider makes a small cut in the abscess to drain the pus. This is usually done under local anesthesia to ensure comfort.
- Antibiotics: Oral antibiotics may be prescribed to help clear up the infection, especially if the abscess is large or if the infection is spreading.
- Pain management: Over-the-counter pain relievers (like ibuprofen or acetaminophen) can help manage discomfort.
7. Complications
If left untreated, abscesses can lead to more severe complications:
- Cellulitis: The infection can spread to surrounding skin and deeper tissues, causing cellulitis, a more widespread bacterial skin infection.
- Sepsis: In rare cases, if the infection spreads to the bloodstream, it can cause sepsis, a life-threatening systemic response to infection.
- Chronic abscesses: Some individuals, especially those with compromised immune systems, can develop recurring or chronic abscesses.
Reference Material
- Mayo Clinic: Provides detailed information about abscesses, their causes, and treatments. Mayo Clinic – Abscess
- American Academy of Dermatology (AAD): Offers insights into skin infections, including abscesses. AAD – Abscess
- National Institutes of Health (NIH): Offers scientific research and data on skin infections and abscess formation. NIH – Abscess